
Operation Smile Rwanda is strengthening local healthcare
Closing the gap: Q&A with Dr Paulin Banguti, one of the just 15 Anaesthetists in Rwanda.
Increase capacity four fold
Anaesthesia is as vital to a surgical procedure as any instrument wielded by the surgeon. As part of Operation Smile’s Global Standards of Care, it’s a medical standard that enables the delivery of the safest surgery and is essential for successful medical outcomes. While this may seem like an obvious standard — if not the most important standard — it reflects a dramatic shortcoming that the Rwandan healthcare system faces.
This densely-populated country of 11.9 million people is served by only 15 nurse anaesthetists and anaesthesiologists.
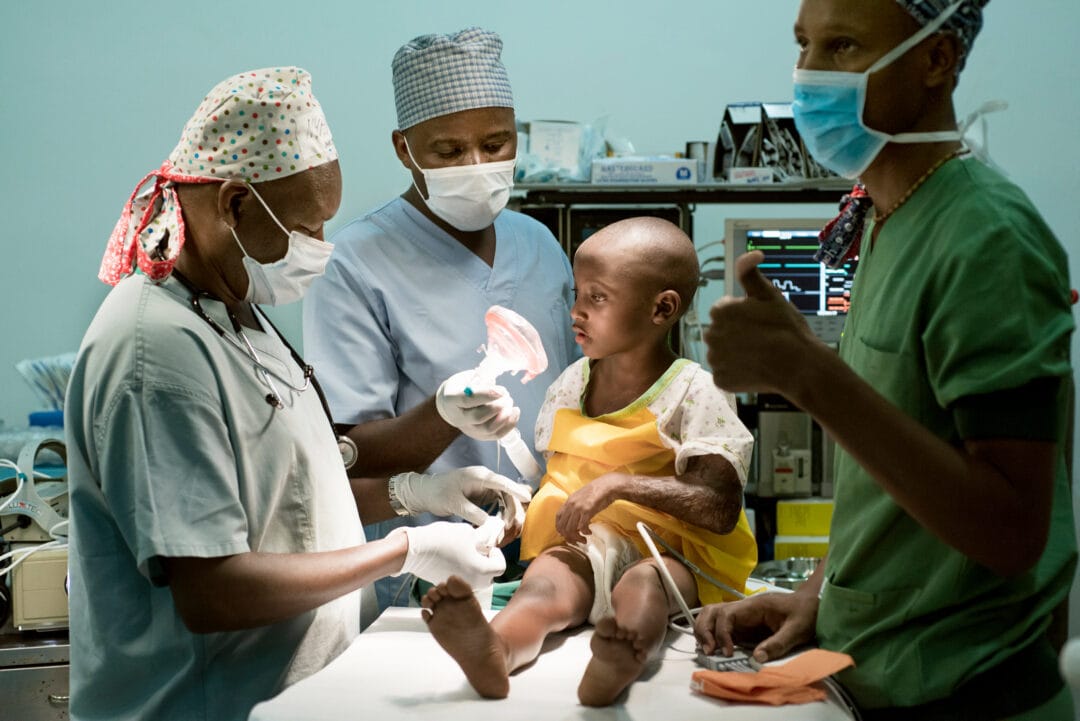
However, Dr. Paulin Banguti, director of the post-graduate anaesthesia programme at the University of Rwanda, is working toward filling this massive void. During the March 2016 Operation Smile surgical training rotation at Rwinkwavu District Hospital, Banguti led a group of anaesthesia residents to observe and learn from volunteer anaesthesiologists from around the world.
“I have appreciated the teamwork spirit. The way the surgeons are communicating, they are very humble,” said Rwandan Dr. Josua Nzarora, a fourth-year anaesthesia resident. “With Operation Smile, everyone respects each other, there is teamwork and things go smoothly and fast.”
Banguti’s goal is ambitious; to train 60 active anaesthesiologists by 2024 before doubling that total by 2030. We caught up with Banguti for more insight into the state of Rwandan anaesthesiology and this groundbreaking educational programme.


Q: What inspired you to shift your focus toward training anaesthesiologists?
A: “After completing my medical training in the Democratic Republic of the Congo, I returned home to Rwanda in 2004 and worked as a general practitioner specialising in maternity. Rwanda launched its first anaesthesiology specialisation programme in 2005 and it really started from the ground-up. There were not enough mentors to teach us, so we were taught by nurse-anaesthetists, who are skilled technicians, but not doctors. There were some ups and downs in the training, which inspired me to offer the best training of residents and anaesthesia practices for the safety of my country.”
Q: How does Operation Smile’s commitment to education align with your vision?
“What’s great is that Operation Smile isn’t bringing us the curriculum or the programme to adopt. When my residents join this programme, they continue to follow our curriculum while learning which aspects to adjust. Operation Smile is partnering with us to achieve the goals we have set and that is why we think it’s sustainable — because with or without them, we have a goal to achieve. That’s the benefit of working with Operation Smile, they don’t come in and say, ‘Destroy whatever it is you have, we have a new machine.’ They’re just continuing what we started and strengthening it.”
Q: What are the challenges you face in retaining Rwandan anaesthetists?
A: “You are touching on one of our biggest problems; it’s brain drainage. Since there are only 15 nurse anaesthetists and anaesthesiologists for 11.9 million people, some become exhausted and think, “I’d rather leave this country to go work less,” at the same or even a lesser salary. If you increase the inflow of anaesthetists, it will create a balance of those sharing the workload. With that improvement in the quality of their lives, they can feel like it’s better to stay in Rwanda. We need to grow the number of anaesthetists so that everyone can work closer to 45 hours per week and have time for social and family lives.
“What’s great is that many Rwandans now believe in their country. It’s what makes us believe we can have many anaesthetists. The strength of our country are young people who believe they can create a new story of a new Rwanda. We even have a song which talks about making it a paradise both in Africa and the whole word. I think that is the ideology that is inspiring many people to do the same as the leaders are doing.”
Q: Do you feel like this style of training has long-term potential?
A: “Yes. The University is trying to extend training beyond Rwanda’s three teaching hospitals and into the district hospitals where residents there would have the opportunity to learn. If we can perform missions in many different hospitals, the residents will benefit and we can build toward sustainability. I see the impact in three different ways; clinical, academic and administrative. In addition to the technical, clinical training, the residents also learn the academic side of training, meaning they can discuss techniques, become teachers and share the knowledge. Administratively, they learn how to work with pharmacists and logisticians to prepare, conduct and evaluate a mission. We hope to take what we have learned from Operation Smile and one day repeat what they have done for us.”
Teaching to fish
There are more than 11.9 million people living in Rwanda. For the entire population, there are only 2 plastic surgeons. We are working to train more plastic surgeons locally, so patients can have timely access to surgery they deserve.
Cleft care in Rwanda since 2010
